Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Cystic Fibrosis
Condition Basics
What is cystic fibrosis (CF)?
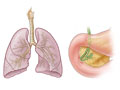
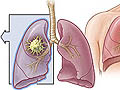
Cystic fibrosis (CF) is a common genetic disease that causes mucus in the body to become thick and sticky. The mucus builds up and causes problems in many of the body's organs, especially the lungs and the pancreas. People who have CF can have serious breathing problems and lung disease.
What causes it?
CF is caused by a change, or mutation, in a gene. The changed gene is passed down in families. To pass on this disease, both parents must be carriers of the changed gene.
What are the symptoms?
Some common symptoms in a baby who has CF include a blocked small intestine, breathing problems, not growing or gaining weight even with a good appetite, salty skin, and diarrhea. Other symptoms in children may include clubbing (rounding and flattening) of the fingers and growths in the nose or sinuses.
How is it diagnosed?
Babies are tested for CF right after birth. The doctor may also notice the signs of the disease during a routine exam. If your child has a positive screening test or symptoms of CF, the doctor will order a sweat test and a genetic test.
How is CF treated?
After a child is diagnosed with CF, a team of health professionals will build a treatment plan. The plan is based on the child's specific health problems. Following a treatment plan will help your child live a longer, healthier life.
A personal treatment plan will quickly become part of your child's daily routine. It will include airway clearance techniques (ACT), medicines, a fitness plan, and nutritional therapies.
Regular visits with the team involved in your child's care are important. Lab tests can help the doctor know how serious the disease is and how it is affecting your child's body.
Some treatments are still being tested and developed. Talk to your doctor about clinical trials and new treatments.
The best treatment available is often found at cystic fibrosis care centers. These centers address medical, nutritional, and emotional needs. Contact the Cystic Fibrosis Foundation at www.cff.org to find one.
Cause
CF is caused by a changed (mutated) gene that a child inherits from both parents. The changed gene causes problems with the way salt and water move in and out of the cells that make mucus. This causes the mucus to be thick and sticky. This glue-like mucus builds up and causes problems in many of the body's organs, especially the lungs and the pancreas.
Many people don't know they have the changed gene.
What Increases Your Risk
CF is a genetic condition. It is an autosomal recessive disease. This means that to get the disease, you must inherit the changed (mutated) gene from both parents. Keep in mind:
- If a person inherits the changed gene from only one parent, they will not get CF but will be a carrier of the disease. Carriers may pass the changed gene on to their children.
- If you are planning to get pregnant, talk to your doctor about having a genetic test to find out your chances of having a child with CF.
Learn more
Symptoms
What are the symptoms of cystic fibrosis (CF)?
Symptoms of CF are usually caused by the production of thick, sticky mucus throughout the body. The symptoms aren't the same for everyone.
Common symptoms in a baby who has CF include:
- A blocked small intestine at birth. This prevents the baby from passing stool.
- Very salty sweat or skin.
- Diarrhea.
- Not growing or gaining weight the way that other children do.
- Breathing problems, lung infections, a cough that does not go away, and wheezing.
Other symptoms may also develop in childhood, such as:
- Clubbing (rounding and flattening) of the fingers.
- Rectal prolapse. (Part of the rectum sticks out from the anus.)
- Growths (polyps) in the nose or sinuses.
What Happens
CF causes mucus in the body to become thick and sticky. The mucus buildup can cause problems in many of the body's organs and systems. These include:
- Lungs and respiratory system. People with CF have thick and sticky mucus that traps bacteria. This causes lots of lung infections and often causes permanent lung damage. Bronchiectasis, which is caused by long-lasting airway inflammation, is common.
- Pancreas and digestive system. Mucus can interfere with how the pancreas and liver work. In the pancreas, this can make it hard for the child to absorb nutrients from food. Some people develop diabetes.
- Sweat glands. You may notice that your child has unusually salty skin. CF can cause a person to become easily dehydrated or to have very low salt levels.
- Reproductive organs. The male reproductive system in someone who has CF usually does not have a vas deferens. This means that semen does not contain sperm. Having CF also may make it difficult to get pregnant.
- Skeletal system. People who have CF may have weaker bones than other people. This is because their bones contain lower levels of minerals. Weakened bones can lead to bone fractures or osteoporosis. CF can also cause swollen or painful joints (arthropathy or arthritis). These problems are more common in adults than in children.
Life expectancy
The life expectancy for people with CF has been steadily increasing. Because of newborn screening, many babies with CF are diagnosed before they develop symptoms. Early diagnosis and personalized treatment can help them feel better and live longer.
When to Call a Doctor
It's important to diagnose and treat CF early. Call your doctor if your child:
- Often has lung infections (pneumonia), colds, a cough, shortness of breath, or wheezing.
- Coughs up mucus that contains blood.
- Doesn't gain or stay at the same weight.
- Has smelly, large, greasy stools or diarrhea.
- Tires easily during activity.
- Has rounded, flat fingertips (clubbing).
Call your doctor if your child who has been diagnosed with CF gets worse in any way. Typically, this is when your child:
- Has increased coughing or has a cough that is getting worse.
- Has new or worse wheezing.
- Has more trouble breathing than usual.
- Has lost weight or isn't gaining weight, for no clear reason.
- Is having symptoms that you and your doctor have discussed as being more serious problems.
Exams and Tests
A medical history and a physical exam are often the first steps in diagnosing CF. This is followed by screening or lab tests.
The diagnosis of CF requires one of the following:
- Symptoms of CF
- A parent, sibling, or child who has CF
- A positive newborn screening test
Also, there must be at least one of the following:
- A genetic test showing that a person inherited a changed gene (known as the CFTR gene) from each parent.
- A positive sweat test showing a higher-than-normal level of chloride in sweat.
- An abnormal nasal potential difference test. This test uses electrodes on the lining of the nose to see how well salts flow into and out of cells.
Early detection tests
Both newborns and adults can be tested for the changed (mutated) gene that causes CF. These tests include:
- Newborn screening. This checks levels of a digestive enzyme from a blood sample. Some newborns may also have a genetic test.
- Carrier screening. This uses a sample of blood, saliva, or cells from inside the mouth. A standard test looks for the most common changes in the gene. An expanded test looks for more changes. Having the gene change means a parent can pass it along to their child.
- Prenatal testing. This is done during pregnancy. This uses a sample of amniotic fluid from amniocentesis or a tiny piece of placenta removed during chorionic villus sampling.
Learn more
Treatment Overview
After your child is diagnosed, a team of health professionals will work with you to build a treatment plan. The plan is based on your child's specific health problems. It may include respiratory therapy, medicines, a fitness plan, and nutritional therapies. Following this plan, along with getting regular medical care and taking steps to reduce infection, can help your child lead a longer, healthier life.
Some treatments are still being tested and developed. Talk to your doctor about clinical trials and new treatments.
The best treatment available is often found at CF care centers. These centers address medical, nutritional, and emotional needs. Contact the Cystic Fibrosis Foundation at www.cff.org to find one.
Doctor visits and vaccines
Regular visits with the team involved in your child's care are important. Your doctor will want to make sure that your child eats well and gains weight and grows at a normal rate. The doctor will record your child's weight, height, and head size. This lets the doctor keep track of how your child develops over time.
Lab tests can help your doctor know how serious the disease is and how it is affecting your child's body.
Your doctor will ask you about your child's immunizations. The doctor will schedule any shots that are needed. Children with CF should have all the recommended shots, plus pneumococcal shots.
Respiratory therapy
Respiratory therapy is any treatment that slows down lung damage and improves breathing.
People with CF have thick and sticky mucus that traps bacteria. This causes lots of lung infections and often causes permanent lung damage. The focus is to reduce infection and get rid of mucus to keep the lungs healthy. Medicines may be used to control the amount and thickness of mucus.
Other ways to help remove mucus from the lungs involve airway clearance techniques (ACT). These include coughing and breathing exercises, wearing a percussive vest, and using positive expiratory pressure (PEP) devices.
Digestive therapy
This treatment works to replace certain digestive enzymes. It helps to make sure the body absorbs all the vitamins and minerals it needs. This treatment also can prevent or treat intestinal blockages. It involves:
- Digestive enzyme replacement therapy. This therapy helps the intestines absorb nutrients from food.
- Nutritional therapy to help replace lost nutrients. This may include taking vitamins; eating high-calorie, high-fat foods; drinking nutritional drinks; getting fed through a tube in the stomach; and, in some cases, receiving intravenous nutrient supplementation.
- Preventing intestinal blockages with stool softeners (to avoid constipation) and enemas.
Learn more
Watch
Self-Care
Caring for your child
- Give your child foods that meet your child's special nutritional needs. A dietitian can help you plan meals.
- Encourage your child to exercise. It can make your child feel better. Talk to the doctor about ways that your child can be active.
- Encourage your child to drink a lot of fluids. People who have CF need extra fluids. Ask the doctor how much fluid your child needs.
- Follow your doctor's directions to keep your child's airway clear.
- Make sure your child gets all the recommended childhood vaccines, plus the pneumococcal vaccine.
- Keep your child away from smoke. Do not smoke or let anyone else smoke around your child or in your home.
Handling the challenges of CF
You and your child will struggle at times with this illness. But having a good attitude and a lot of support will help both of you cope.
- Focus on your child's strengths. Let your child know that you love and believe in them.
- Give your child some responsibility for their own care. Children who have a say in their treatment often stay healthier.
- Learn about the disease. This will help you figure out what you can do to help your child.
- Do the best you can, and know that you can't control everything.
Self-care for adults who have CF
- Take your medicines and vitamins.
- Do treatments to clear your airways.
- Get pneumococcal and yearly flu vaccines. Stay up to date on your COVID-19 vaccines.
- Have those close to you get vaccines as well.
- Drink plenty of fluids. If you have kidney, heart, or liver disease and have to limit fluids, talk with your doctor before you increase the amount of fluids you drink.
- Follow the meal plan created by your dietitian.
- Get aerobic exercise to help loosen mucus and improve oxygen flow. Talk to your doctor about what is best for you.
- Do not smoke or allow others to smoke around you. If you need help quitting, talk to your doctor about stop-smoking programs and medicines. These can increase your chances of quitting for good.
- Do not vape.
- Avoid alcohol, marijuana, and other drugs. They can make it harder for you to manage your care.
- Join a cystic fibrosis (CF) support group. And spend time with those close to you.
- Think about joining a clinical trial of a new CF therapy. Many new medicines are being studied for cystic fibrosis.
Learn more
Watch
Getting Support
If you are caring for a child who has special health care needs, it may be helpful to get support for yourself.
Think about joining a support group in your area, or even online. Support groups can be a source of emotional support for you and your child. These groups can help you connect with other parents who have a child with the same condition. They can also help you learn what resources you can find in your area.
You may also find counseling useful. A counselor can help you understand and manage the wide range of emotions you may feel.
Learn more
Watch
Medicines
Medicines for CF help keep the lungs as healthy as possible, reduce and control mucus in the lungs, and replace digestive enzymes. There are also medicines that can improve lung function for those with certain gene changes.
Some medicines cost a lot, but there may be programs to help pay for them.
Medicine choices
- Medicines to treat infections. These include:
- Antibiotics (such as azithromycin, ciprofloxacin, or tobramycin).
- Medicines to open airways in the lungs or keep them open. These include:
- Bronchodilators (such as albuterol or levalbuterol). They can make breathing easier. They may also make it easier to cough up mucus.
- Medicines to control mucus. These include:
- Dornase alpha, also called DNase. It's used to thin mucus in the lungs.
- Saltwater solution (hypertonic saline). This is sometimes used to help clear mucus from the lungs.
- Medicines to reduce inflammation. These include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) (such as ibuprofen).
- Corticosteroids (such as fluticasone or beclomethasone).
- Medicines to replace the effect of digestive enzymes. These include:
- Enzyme replacement therapy (such as pancrelipase or pancreatin).
- Medicines that improve lung function and other symptoms. These include:
- Medicines called CFTR modulators. People who have CF have changes in the cystic fibrosis transmembrane conductance regulator (CFTR) gene. Medicines such as elexacaftor, ivacaftor, and tezacaftor can help people who have certain types of CFTR changes. Having a gene test can show if these will work for you or your child.
Learn more
Surgery
Surgery may be needed to treat problems from CF. These procedures may include:
- Lung transplant. It may be done for people who have severe lung disease. Not everyone is a good candidate for a lung transplant.
- Chest tube drainage and possible thoracoscopy. This is done to treat a collapsed lung (pneumothorax).
- Repair of an intestine that has collapsed inside itself or removal of a bowel obstruction.
- Removal of nasal polyps or endoscopic sinus surgery.
If a child has CF and isn't able to get all the nutrients they need from food, a feeding tube may be placed in the child's stomach.
Learn more
Watch
Respiratory Therapy
CF causes mucus to become thick and sticky, which can clog the lungs and cause serious problems. You can help your child maintain lung function and avoid problems from mucus buildup and blockage by doing airway clearance techniques. As your child gets older, they'll be able to do this on their own.
Airway clearance techniques (ACT) include special breathing and coughing exercises. It may involve using postural drainage and percussion. An older child or adult may use a percussive vest or use a positive expiratory pressure (PEP) device. These all help with clearing mucus from the lungs.
Your child's care team will make a personal treatment plan that includes ACT. These therapies are one part of a larger treatment plan to help keep your child's lungs clear.
It is important for your child to visit their doctor regularly and make any needed changes in treatment.
Learn more
Related Information
Credits
Current as of: October 6, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 6, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2026 Ignite Healthwise, LLC.